Researchers at the University of Maryland, Baltimore (UMB) are attacking a pressing and perplexing medical problem: What causes chronic pain? How to ease it? How to predict — and prevent — its occurrence?
In collaboration through the University of Maryland Center to Advance Chronic Pain Research (CACPR), scientists are seeking to address these key issues related to pain. Importantly, they also are doing so in response to a growing national crisis of opioid addiction disorders that has been amplifed by the COVID-19 pandemic. The center’s mission is to cultivate and expand the multidisciplinary pain research portfolio at UMB with the overarching goal of improved patient care and quality of life.
This pain research matters greatly to chronic pain sufferers, such as cancer survivors whose treatment comes with debilitating tradeoffs, and to victims of addictive painkillers.
In 2018, in response to the growing national opioid crisis, the National Institutes of Health (NIH) launched its Helping to End Addiction Long-Term (HEAL) Initiative. A survey showed that during 2018 alone, more than 10 million people misused prescription opioids. The yearly death toll by June 2020 stood at 48,000 due to synthetic-opioid overdose.
The $1 billion federal initiative accelerated the search for nonaddictive therapies and, importantly, the need to better understand and manage pain.
“Pain is actually beneficial,” says Man-Kyo Chung, DMD, PhD, who is CACPR’s co-director. It prevents harmful injury; for example, children learn not to touch a hot stove. But sometimes the mechanisms go awry. Some people lack pain sensitivity because of a gene mutation. “And their life is miserable,” he says.
Chronic Pain Is a Disease Afflicting 1-In-5 Adults
Experts agree that individuals find themselves beset by pain for reasons known and sometimes unknown. “Chronic pain is considered a disease,” says Chung, professor and interim assistant dean of research at the University of Maryland School of Dentistry (UMSOD). The disease afflicts one in five U.S. adults, according to 2019 statistics.
While some current therapies are effective in treating chronic pain, not all are effective for the large number of adults suffering from chronic pain. Those gaps, and a push to avoid opioids, add urgency to scientists’ search for alternative analgesics or ways to deploy the body’s own resources. Chung is among those exploring analgesics; he studies capsaicin, a substance found in chili peppers.
Among those seeking clues within the human body are three professors at the University of Maryland School of Nursing (UMSON). Luana Colloca, MD, PhD, MS, investigates how genetics and a person’s expectations can modulate pain experience and response to treatment in cases of temporomandibular joint disorder (TMD). Susan G. Dorsey, PhD ’01, MS ’98, RN, FAAN, chair of UMSON’s Department of Pain and Translational Symptom Science and co-director of CACPR, and Cynthia L. Renn, PhD, MS ’97, RN, FAAN, search for biomarkers in patients with low back pain.
“We’re capturing patients when they’re having an acute episode,” Renn says of the study with Dorsey. “Is there something that we can identify in these patients that might indicate whether they’re going to go on to develop chronic low back pain? Or will they recover?”
HEAL Research at CACPR
Together, Dorsey and Chung head a center whose prominence has grown as UMB researchers secure multiyear grants, totaling $9.7 million, under the NIH HEAL Initiative. All could help reduce Americans’ reliance on addictive painkillers, and several grants that fund basic, translational, and clinical biomedical research could lead to key discoveries about pain.
What if the body could alert us to pain susceptibility? UMSOD assistant professor Joyce Teixeira da Silva, PhD, associate professor David Seminowicz, PhD, and colleagues have uncovered evidence of a cortical biomarker signature that is predictive. Their grant funds a search to identify at-risk individuals.
It remains unclear how postsurgical patients overcome pain or fail to resolve it. UMSOD assistant professor Ohannes Melemedjian, PhD, aims to spare patients from chronic pain after surgery by validating a certain glutamine transporter as an endogenous treatment. Under another grant, he seeks to identify novel molecular targets to treat chemotherapy-induced peripheral neuropathy. The side effect compels some cancer patients to halt lifesaving chemotherapy.
One medical mystery involves the jaw and the gut. They’re paired in a chronic overlapping pain condition in which TMD sufferers report symptoms consistent with irritable bowel syndrome. Richard J. Traub, PhD, professor and chair of UMSOD’s Department of Neural and Pain Sciences, and Melemedjian are investigating by using brain imaging and other methods.
Pain Perception During Pandemic
UMSON’s Colloca, a placebo expert who also is an inaugural MPower Professor and associate professor in the Department of Anesthesiology at the University of Maryland School of Medicine, has shed light upon the mind’s capacity to shape pain perception in two studies related to the pandemic.
An opportunistic survey conducted online during the 2020 lockdown found that participants who self-reported nonspecific COVID-19 symptoms had higher pre-pandemic depression. “It’s not merely asking, ‘How do you feel?’ Rather, there are structural questions that we use clinically,” she says. Respondents revealed great anxiety. She and co-authors concluded that patients with underlying mood disorders may require more help than they did before the pandemic.
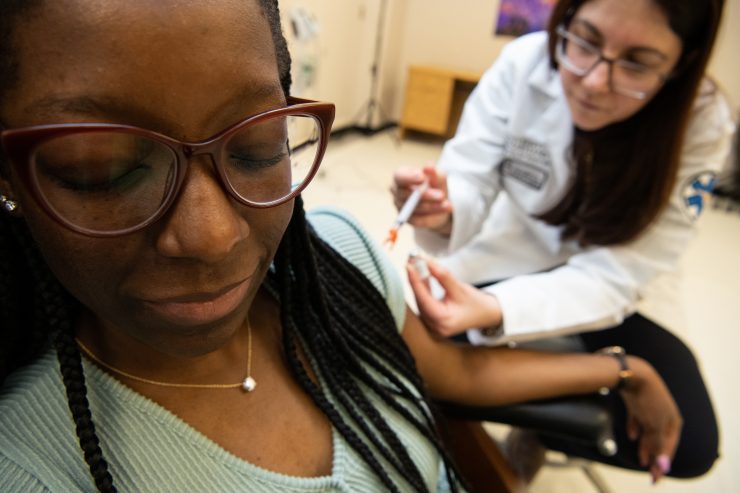
A study with implications for reducing vaccine hesitancy examined negative expectations, or nocebo, the opposite of placebo. Individuals who were looking for trouble found it; they reported greater pain perception such as injection-site soreness.
“We are the first to demonstrate a link between nocebo-related factors and COVID-19 vaccine experienced side effects,” Colloca and colleagues wrote in a letter to the editor of Psychotherapy and Psychosomatics. They suggested strategies to confront nocebo and to curb hesitancy.
Although chronic-pain complexities are daunting, CACPR’s multidisciplinary structure gives its scientists an advantage.
“Our center provides an optimal environment for investigators to really collaborate and develop new research ideas and make progress,” Chung says.